Office Hysteroscopy: Simple set up is the best approach
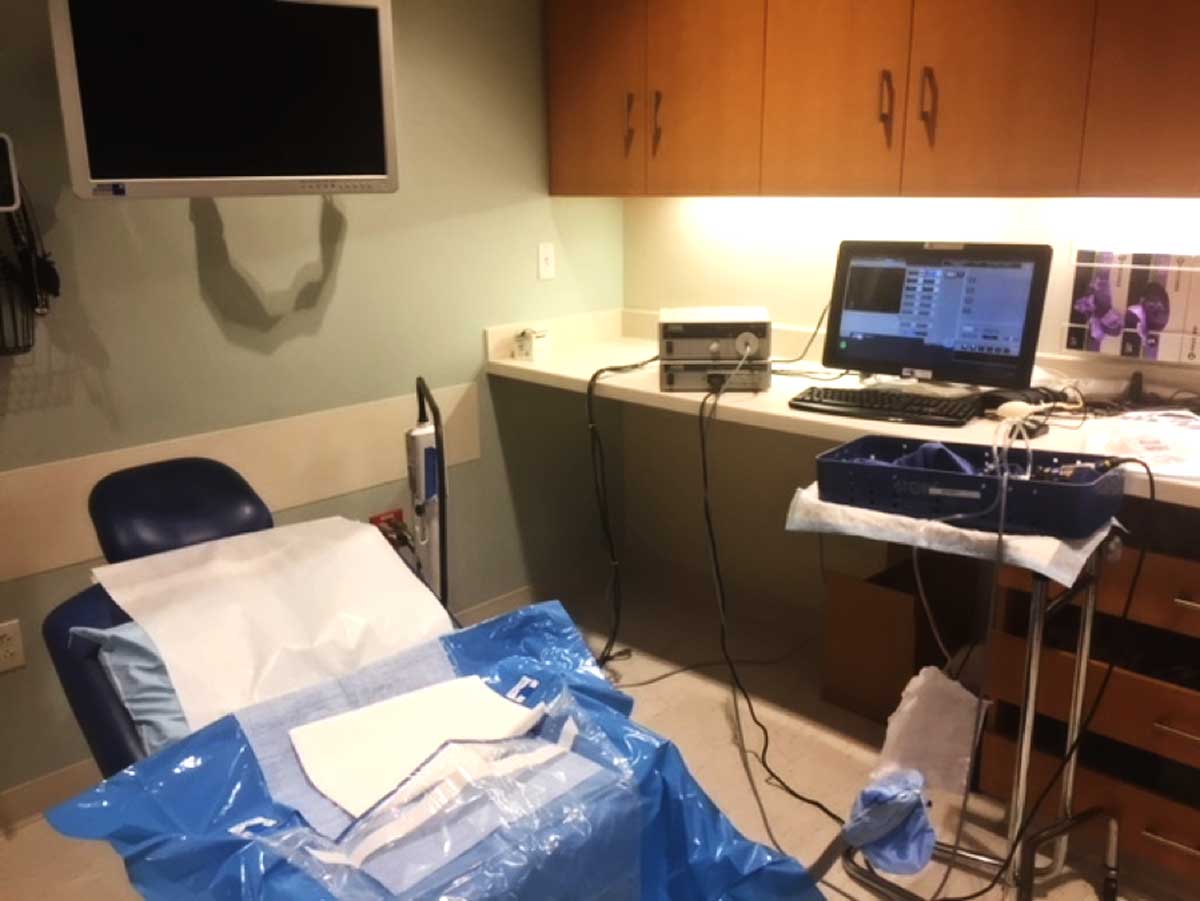
Office hysteroscopy in a basic exam room
In 2018, nearly 100% of practicing gynecologists agree that evaluating the uterine cavity is THE standard of care when treating reproductive age women with abnormal uterine bleeding, women with post-menopausal bleeding, and women presenting with infertility. While saline infusion sonography is an excellent tool for evaluation and should complement direct hysteroscopic visualization, only hysteroscopy performed in the office allows the provider to diagnose and treat intrauterine pathology in one procedure. The question is often raised, “why aren’t 100% of gynecologists offering this office based procedure to their patients?” While I don’t have the magic answer, I do believe that identifying and minimizing barriers is key for greater adoption of office hysteroscopy which directly translates to better care for our patients. Complexity and costs of set up is one of those barriers that can be minimized by a simple approach.
Let’s define what is meant by a simple approach. Simple is defined by performing hysteroscopy safely and effectively in an office setting without the need for general, regional, or intravenous anesthesia. Simple means a patient can potentially have the procedure performed on her initial visit without the need to disrupt her life further with a second visit. Simple means when the patient leaves the office, she can go back to normal activities and work the same day. Simple means there is minimal need to invest in high cost equipment or high cost “procedure rooms” to perform office hysteroscopy. Simple means that no special schedule is needed to perform office hysteroscopy. The exam should not take longer than a typical well visit annual exam and fits in easily to a typical schedule. Simple means that office hysteroscopy can be performed by a single provider and a medical assistant. Simple means that there should be standards in place for efficiently cleaning and sterilizing reusable equipment within 20-30 minutes. Simple means having crises checklists onsite that can be rehearsed should there be a rare medical complication from the procedure. Simple means that office hysteroscopy should be rewarding both professionally and financially for the office based practice.
To achieve simplicity, I have the following recommendations:
- Define your mission.In my practice I routinely perform diagnostic hysteroscopy as well as any procedure I can do with no anesthesia except oral NSAIDs and a very rare paracervical block. These are vaginoscopic procedures that include polypectomy, small myomectomy, metroplasty and lysis of adhesions. These are procedures that can be performed with a continuous flow 5mm OD hysteroscope that has a 5Fr working channel for reusable scissors and tenaculum.
- Make office hysteroscopy convenient for you and your staff.Standardize the set up and use exam rooms within the practice suite. While there is no need for a designated procedure room, a standardize set up for any exam room with a hysteroscope, light source, camera, and monitor is helpful. In our practice, we use 4 different standard exam rooms. We have two rooms in where the hardware is housed and a mobile cart for the other rooms. All we need to perform the procedure is a commercially available packet that contains a collection drape and inflow and outflow tubing as well as a designated pump to provide distention pressure and suction if needed.(Figure 1, 2) The drape system is key to our efficiency since no fluid goes on the floor or on the table and there is minimal time needed for room turnover. Cleaning and sterilization of equipment is done with enzymatic soap and Cidex OPA and allows sterilization to be complete within 30 minutes (Figure 3).
- Minimize frustration.Learn vaginoscopic techniques via online videos and attend regional, national, and international hysteroscopic conferences. Practice in the operating room when the patient is under anesthesia. When you master the technique of performing office hysteroscopy with no speculum, tenaculum, or paracervical anesthesia, it is hugely rewarding and fun. You will soon realize that the speculum initiates anxiety that heightens pain sensation. Most often there is zero discomfort to the patient until the scope passes through the internal cervical os and by that time you are over half way done with the diagnostic procedure.
- Keep the equipment simple.The reimbursement for office hysteroscopy is widely variable in different regions of the country and world. In the U.S., I believe I practice in an area with some of the lowest reimbursement in the country, and still, office hysteroscopy is extremely productive to our practice. We accomplish this by using as much reusable equipment as possible while paying for disposable items that maximize our efficiency. Our telescopes are rod/lens scopes that have lasted over 15 years. The same holds true for our camera and light source. We have upgraded our monitors to flat screens but HD is not necessary. We use reusable 5Fr instruments but only get 10-15 uses out of the scissors before they become too dull to cut. Including our disposable drapes, tubing, and fluid, our simple set up cost approximately $25 – $30 per case. Depending on the procedure, our reimbursement is from $275 – $1400 per procedure. If one were to lease equipment, they would only need to perform 2 cases per month to cover the cost of the lease. Every case beyond that is productive to the practice. My two partners and I perform 15-20 office hysteroscopies a week in our simple office.
In summary, a simple, efficient office set up removes many of the barriers that discourage physicians from providing office hysteroscopy for their patients. A simple set up saves costs while maintaining safety and productivity. Several endoscopic companies have expressed interest in developing products specifically designed for office hysteroscopy. If we had a company that could provide one stop shopping for disposable and reusable equipment and help with physician and patient education, it would enhance the simplicity even further. A doc can only dream!
References
- Salazar CA, Isaacson KB. Office Operative Hysteroscopy: An Update. JMIG August 2017
- Wong M, Miller V. Why you should be performing office hysteroscopy …now. Contemporary OB/GYN.net Sept 27, 2017







