Difficult Case: Abdominal Approach for Retropubic Sling Removal

Last year we have featured cases and articles from AAGL’s Special Interest Groups (SIG) and in this issue, the Urogynecology SIG is in the spotlight! The most difficult case has to deal with Abdominal Approach for Retropubic Sling Removal, pictured in the image below.
Thank you to all the AAGL SIG chairs, vice-chairs, and members – for the informative and timely articles and for supporting this exciting series!
Persistent post-operative pain (PPOP) is a rare complication in the placement of retropubic slings.1 One study reported persistent pain following a retropubic sling placement to be around 10% in comparison to a rate of 32% following a transobturator approach.2 There is robust evidence supporting conservative non-surgical management for PPOP associated with mesh insertion.3 There is little evidence supporting anyone approach being superior. Unfortunately, many physicians are unfamiliar with PPOP, or unsure of how to optimally treat it. When conservative management fails, physicians should only then consider surgical management. Due to the technical difficulty associated with sling revision and/or removal, patients experiencing PPOP after a mid-urethral sling who have failed conservative non-surgical management should be referred to physicians who have expertise and experience with these cases. A laparoscopic approach is feasible, however, it can result in sling material remaining within the abdominal wall itself, which can be problematic. The most ideal approach to ensure removal of all sling material from both the space of Retzius and abdominal wall is through a mini laparotomy.
CASE: A 45 year old female presented with a 3-year history of PPOP since the placement of a retropubic mid-urethral sling in 2017. During the 3 years prior to her presentation, the patient underwent a multitude of evaluations and treatment plans by a variety of medical health professionals. She reported an extensive history of failed conservative methods and had exhausted efforts from relief by multiple pain specialist after steroid injections and local anesthetic failed to provide her relief.
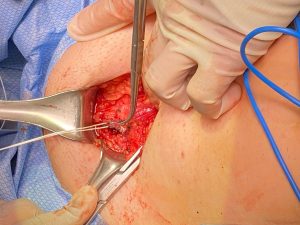
On physical exam the patient had suprapubic tenderness and scar-like tissue texture change in the suprapubic region and a plan was made for surgical revision/removal of pubovaginal sling/mesh. A small (6cm) Pfannenstiel incision was made with scalpel and the incision was carried down to the fascia. The fascia was incised and the underlying pyramidalis and rectus muscle were dissected off sharply. The rectus muscle was then identified and separated down to the level of the pubic symphysis. The underlying muscle was dissected off of the fascia to the level of the space of Retzius. (Image 1)
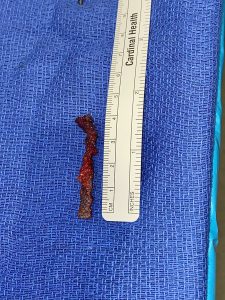
The left arm of the retropubic sling was then visualized only 1 cm medial to midline of the pubic symphysis and just above Cooper’s ligament. With combination of blunt and sharp dissection, the mesh was then separated from the underlying and surrounding tissue. The mesh was then localized and followed up through the fascia and to the underlying subcutaneous fat where the mesh was identified. The mesh was then separated and brought up from the fascia into the subcutaneous area. The subcutaneous end of the mesh was then identified and removed from the patient. A 4 cm segment of the retropubic sling was then removed in its entirety from the level of the pubocervical fascia. (Image 2)
The removal of the poorly placed arm of the sling provided pain relief for the patient without compromising the effectiveness of its purpose for midurethral stability. At 2 weeks and 6 weeks out the patient was pain-free without any recurrent urinary incontinence.
- Duckett J, Baranowski A. Pain after suburethral sling insertion for urinary stress incontinence. Int Urogynecol J. 2013 Feb;24(2):195-201. doi: 10.1007/s00192-012-1863-3. Epub 2012 Jul 3. PMID: 22752013.
- Cetinel B, Tarcan T. Management of complications after tension-free midurethral slings. Korean Journal of Urology 2013;54:651-9.
- Charles W. Butrick Persistent postoperative pain: Pathophysiology, risk factors, and prevention Female pelvic medicine and reconstructive surgery V22 N5 Sept/Oct 2016.